First and last name: C.N.
Age: 87 years
Diagnosis: Bilateral lymphedema in the lower limbs, severe right knee osteoarthritis and heart failure
Bilatheral Lymphedema
- Home
- Bilatheral Lymphedema
The patient has had lymphedema for about 15 years and has never been treated with MLD. She previously worked as a laundress for about 15 years, a profession that forced her to remain standing throughout the workday. She then worked as a janitor in an apartment building until retirement. She has had four pregnancies.
Progressive deterioration of ambulatory control. Has not left the house for about three years. At night she sleeps very little, given the presence of osteoarthritis in her right knee.
The patient reported that sometimes small blisters from which liquid comes out form on the legs which then heal spontaneously leaving small depressions in the skin. When she feels discomfort in her legs she applies old elastic bandages which have lost their elasticity, but which give relief.
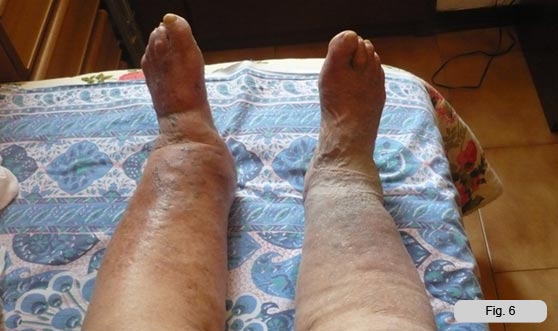
The feet are not edematous, presumably because she uses footwear.
Lasix 25mg, 2 in the morning- Lanoxin 250mg, 1 in the morning- Eutirox 5mg, 1 in the morning-Bisoprolol 1.25mg, 1 in the morning- Coumadin 5mg, 1 daily- Kolibri, 1-2 daily.
The patient is lucid, cooperative. She walks with difficulty dragging a chair.
Uses slippers that require her to drag her feet reducing the pumping action of the calf muscle and squeezing action on the sole of the foot.
Difficulties in passing from a sitting/ standing, sitting/ supine positions and vice versa is also due to the weight of the lower limbs.
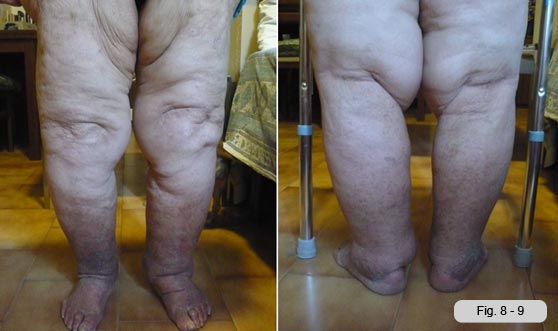
Lower limb edemas are hard, non hyperthermic, shiny skin, tight and intact.
The measurement of the circumference of the lower limbs confirms the visual impression that the right limb is the most edematous. (Tab.1)
On 12/04/11 the patient is evaluated by the physiatrist who prescribes an arterial and venous Doppler ultrasound.
The examination is viewed by the GP who is also the patient’s cardiologist. The cardiologist believes that there are no absolute contraindications to treatment with MLD and bandaging as the ultrasound shows no underlying conditions, and heart failure is currently well compensated by drug therapy.
We agree on a gradual onset with no bandaging, treatments spaced out and monitoring of the clinical condition of the patient.
The treatment is carried out at the patient’s home in ADI.
• MLD + bandaging one limb at a time starting from the more edematous limb (right)
• exercises for active mobilisation of lower limbs
• rehabilitation of gait
• evaluation and prescription of walking aid
• evaluation and prescription elastomeric compressive stockings
I began with two treatments using only MLD at an interval of 5 days after the other involving family members to monitor a possible imbalance in the hours following the treatment.
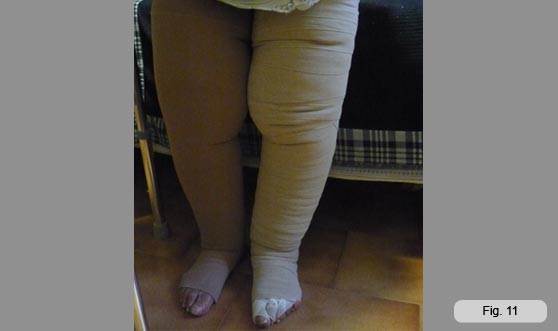
After verifying that the MLD was well tolerated I began to bandage the limb with a multilayer bandage up to the thigh.
The frequency of treatment was three times per week.
After the third bandage I was forced to temporarily suspend bandaging because the day after the fifth treatment the patient, despite feeling pain did not take off the bandages. This caused an increase in edema in a localised area of the leg that was resolved with the MLD.
Given the poor reliability of the patient, I began to bandage it with a well tolerated one-layer bandage.
However, the pain and the increase in the edema kept on recurring until I realised that the patient was rolling tights around her thigh in order to prevent the bandages from falling off.
After 14 sessions a technician took measurements for the creation of a 2nd class graduated compression stocking.
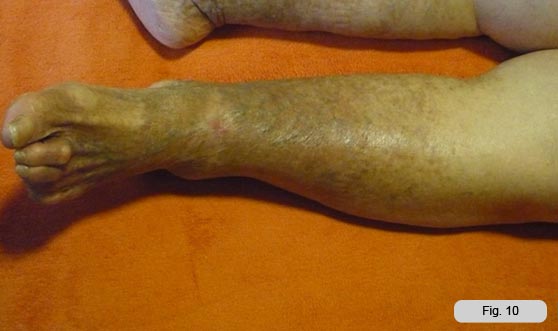
I continued the treatment until the delivery of the stocking that the patient had learned to wear themselves resulting in further reduction of the edema. At the end of the treatment the limb was less edematous, softer, less painful and the patient never presented with episodes of lymphorrhoea. The skin was clearer.
Simultaneously to the treatment with MLD a walker was prescribed which allowed the woman to walk with more safety in the home also lightening the load on the painful knee because of severe knee osteoarthritis.
And the patient was asked to stop using the slippers and rehabilitation on correcting gait pattern was arranged.
The patient was taught some simple motion exercises for the lower limbs and isometric contractions that she began to perform daily.
Because of the initial caution and delays during therapy, the treatment of the right lower limb finished in early summer (06/06/2011).
Not being able to ensure continuity in the summer, in agreement with the physiatrist, it was decided that treatment of the other limb would be postponed until after the end of summer.
The patient complains of difficulty in walking for the pain in her right knee. The stocking is well tolerated even if there is a little redness at the instep probably due to the fact that the patient spends most of the day sitting.
The left leg is edematous The skin is shiny, taut and reddened, so the geriatrician prescribes a cortisone ointment for local use. The hyperemia resolves in a few days.
The presence of lymphorrhoea from a small wound, in the front of the leg is also noted, which is struggling to heal. Two other small wounds have recently closed, forming a small crust.
I started treating the limb only with MLD without bandaging because the presence of lymphorrhoea. The small wound was cleansed with Betadine. After two sessions of MLD, the lymphorrhoea has stopped and the wound closed, forming a small crust.
The treatment is continued at a frequency of three times a week.
At this point I put a one-layer bandage and, seeing as it was well tolerated from the beginning, I added another layer bandage after getting a good edema reduction over 10 sessions.
I subsequently had to suspend the use of bandage for the appearance of redness at the instep. Even in this case, the patient, while feeling pain at that point, did not want to cease with bandaging.
The momentary interruption of the bandaging treatment, but not of the MLD, caused an increase in limb edema, particularly of the leg as shown by measurements of 10/10/11 forcing me to postpone the creation of a compression stocking.
On 18/10/11 a 2nd class graduated compression stocking was prescribed. Since the right stocking, prescribed previously, has caused reddening of the instep, the technician evaluated the situation and decided to insert a special feature at 90° to the ankle to decrease pressure at that point.
The stocking was delivered on 22/10/11.
On the weekend following the delivery of the stocking, the patient was bedridden with acute lumbago. She remained in bed for two days, getting up only for short periods and wearing the stockings during the day. This has resulted in the appearance of redness on the instep of the foot to the increase due to the compression exerted by the stockings in the supine position.
I advised the patient to remove the stockings and keep her limbs in a sloping position when she stayed in bed. For the reddened area the GP prescribed the application of Colladermina ointment with gradual resolution of the problem.
After the acute phase of low back pain had subsided I started with the mobilisation of the lower limbs and rehabilitation of the gait.
She quickly regained security, speed and agility when walking.
These improvements have allowed her to leave the house and to walk out of the home for medium/ long periods of time.
The limbs were softer.
By wearing the stockings daily and increasing the amount of movement, there was a further reduction of the edema of the lower limbs.
The patient was discharged on 02/12/2011 with the recommendation to replace the stockings every nine months.